What do thrush, candidiasis, mycosis and yeast have in common? Well, they’re all words that can be used to describe the presence of fungi! That said, how can we conclude that fungi are present, and more importantly, what should we do when they are?
Although this situation may seem alarming to you, rest assured that the presence of fungi in a baby aged two months or less is very, very common. We live with fungi in our environment, and it’s a common yeast in humans. The problem is when they settle in the wrong place, causing discomfort in babies and nursing mothers.
Types of infections
There are two types of infection that can occur in babies;
- infection acquired in utero or through the vaginal canal at birth, known as congenital candidiasis
- infection acquired after delivery, known as neonatal candidiasis. In the latter case, it’s certain that the moisture in the diaper, combined with the alkaline pH of the baby’s urine, favors the development of candida infection.
Recognizing a fungal infection
How can you tell it’s fungus?
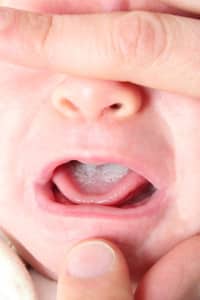
Parents, and even many caregivers, will often tell you that your baby has thrush simply by looking at his tongue. WRONG! Breast-fed babies often have white tongues, without having fungus!
However, in the case of candidiasis, white patches can be seen on the inside of the cheeks, and between the gums and lower lip. These patches are also reminiscent of cottage cheese.
Yeast contamination occurs via the mouth, then travels down the intestinal tract to the anus. And it’s often from here that the presence of fungi is most noticeable: little bright-red or white pimples around the anal opening. These are known as satellite lesions, and tend to enlarge their perimeter, creating significant redness (diaper rash). These pimples (or sores on the buttocks and/or vulva) cause burning sensations when urine and feces come into contact. Baby will let you know of his discomfort, and will cry as a result.
Breast-feeding mothers
In the case of the breast-feeding mother, the following may be noted:
A sensation of pain or burning in the nipples, without seeing anything in particular on her nipples;
Wounds on her nipples that do not heal;
reddened nipples, as if irritated.
One thing’s for sure: if the baby has fungus on its bottom, it also has fungus in its mouth, and the mother is surely contaminated too. That’s why you should always treat the mother if you find fungus on the baby. Otherwise, recontamination is likely, and treatment of the baby alone is therefore ineffective. The mother must be treated, even if she has no symptoms.
Do you suspect the presence of fungi? Don’t hesitate to consult us! The sooner you act, the easier it is to treat the fungus!
 Treating mycosis
Treating mycosis
Prevention is key!
When you start breastfeeding, and throughout the process, it’s important to adopt a good latch to avoid injuries on the mother’s side at all costs. Such injuries (broken skin, irritated nipples) could open the door to fungus contamination.
Treatments for babies
When faced with the presence of mycosis, several actions must be taken:
- Wash pacifiers, soothers and all toys that baby puts in his mouth;
- Avoid moisture as much as possible by changing baby’s diaper often.
- When changing diapers, dry the buttocks and genitals thoroughly. Then apply an antifungal cream (e.g. Canesten® or Monistat® (miconazole). These creams are available over the counter at your pharmacy) in a thin layer, 3 times a day for 10 days.
- Even if the symptoms disappear before the end of the treatment, make sure you maintain the treatment for 10 days, otherwise the fungus could quickly return.
- If the redness is very severe and swelling is present, it’s best to use Monistat® cream, as it also contains an anti-inflammatory. In the case of very severe redness, the antifungal cream can be rubbed in first, followed by a barrier cream (e.g. Zincofax®) to prevent repeated irritation caused by urine and feces coming into contact with the lesions.
Treatments for breast-feeding mothers
If you’re a breast-feeding mother, you’ll need to treat your nipples.
To do this :
- Apply an antifungal cream such as Canesten® or Monistat® (your doctor may also prescribe another cream ((e.g.: magistral cream)) or Jack Newman’s triple cream) to your nipples 3 times a day for 10 days.
- Here too, treatment must be continued for the full 10 days, even if symptoms seem to dissipate before the end of the treatment.
The cream should be applied before and after each feeding. Before, so that the baby sucks your nipples with the cream on, to get some in his mouth and help treat the fungus there, and after the feed for you. The cream will work to treat your nipples and prevent recontamination. - If your mouth is affected, a syrup containing Nystatin may be prescribed. Ask your doctor, nurse or pharmacist.
If you experience symptoms of itching or burning during urination, you can also use Monistat® cream as a vaginal treatment. If, despite this treatment, symptoms increase or remain unchanged after three days, it’s best to consult a doctor.
Caution! As of 2019, Health Canada recommends that gentian violet (crystal violet), regardless of presentation, no longer be used on pregnant women or babies, as it is recognized as a potential cancer risk agent.
Marie Fortier
The Baby Expert
Updated article : April, 2025.
Here are other articles related to baby care :
- Postnatal Baby Care
- Heat and Cradle Cap (in french only)
- Baby Colic
- Baby and Hiccups
- Our Baby is Tanned
Related videos:
References :
-
INSPQ. (2025). Muguet dans la bouche. Repéré le 1er avril 2025 à https://www.inspq.qc.ca/mieux-vivre/sante/problemes-sante-courants/muguet-bouche#:~:text=Le%20muguet%20est%20une%20infection,des%20l%C3%A8vres%20et%20des%20joues
-
CIUSSS MCQ. Fiche d’information sur le traitement du muguet. Repéré le 1er avril 2025 à https://www.ciusssmcq.ca/telechargement/3401/ordonnances-collectives-maskinonge-oc-m-3-fiche-d-information
-
Centre Alima. (2024). Peut-on traiter le muguet avec des remèdes naturels? Repéré le 1er avril 2025 à https://centrealima.ca/fr/ressources/parents/allaitement/gestion-des-defis/peut-on-traiter-le-muguet-avec-des-remedes-naturels
-
Société canadienne de pédiatrie. (2024). Les antifongiques pour traiter des mycoses pédiatriques courantes dans un contexte ambulatoire. Repéré le 1er avril 2025 à https://cps.ca/fr/documents/position/les-antifongiques-pour-traiter-des-mycoses-pediatriques-courantes-dans-un-contexte-ambulatoire
-
Santé Canada. (2019). Santé Canada met les Canadiens en garde contre le risque de cancer associé au violet cristallisé. Repéré le 1er avril 2025 à https://recalls-rappels.canada.ca/fr/avis-rappel/sante-canada-met-canadiens-en-garde-contre-risque-cancer-associe-au-violet-cristallise


