Updated article : September 2023.
Hello Parents,
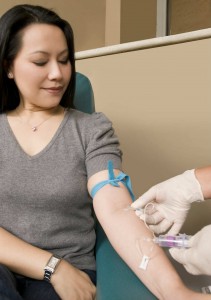
At the start of your pregnancy monitoring, your health professional (nurse, doctor or midwife) will request different tests to evaluate your general health and the health of the future baby. The goal is to quickly act if something is off to ensure that the pregnancy goes well, the baby develops well. You will go through different tests – blood tests throughout the pregnancy, ultrasounds, measurements of your stomach (fundal height), your weight, blood pressure, urine tests and much more…
In this article, I will focus on blood tests at the start of pregnancy.
They are often prescribed during your first monitoring visit taking place between the 7th and 12th week of pregnancy. In Quebec, the blood tests required are pretty standard and are in line with recognised good practices guides. I will talk about the majority of parameters usually requested by your health professional and explain why they are essential for a pregnant woman and her baby. I will also try to simplify as much as possible so you can understand what I am saying, but I will have to use biochemical terms due to the type of issue I am discussing.
Here is a description of each blood test requested:
- Full Blood Count
- Blood type and RH (- or +)
- Search for antibodies
- Toxoplasmosis
- Infectious syphilis (VDRL)
- Screening test for gestational diabetes
- Obesity Evaluation
- Hemoglobin Electrophoresis
Full Blood Count:
A full blood count is a term used to designate a series of specific elements, more than a dozen, associated with your blood and its components. For example, red blood cell count (which transports iron), leucocytes (which help defend the body), plasma volume, etc.
Each element contained in the blood count is essential and will be evaluated to ensure the right measurement and avoid potential consequences.
Why?
Having this data at this point of the pregnancy allows health professionals to act rapidly if there are deficiencies, such as anemia (low iron levels), and recommend higher supplements than usual for the mother. This is to maintain the balance in the dosage of blood elements to optimise the mother’s general health and promote the full development of the baby
Blood Type and RH (- or +)
Each person has their own blood type – A, B, AB or O. When a woman is expecting a baby, it’s important to know:
- Her blood type in case of emergencies or blood transfusions
- Her rhesus (RH) which can either be positive (+) or negative (-)
Why?
For the baby, the mother’s blood type (A, B, AB or O) isn’t a problem because there are two independent blood circulation. On the other hand, RH- can cause problems during pregnancy and for the baby. When a mother is RH+, there’s a rhesus molecule on the surface of the red cells. When negative, there are no molecules.
When the mother has RH+, there shouldn’t be blood problems because the father’s blood doesn’t affect the inter-placenta links between the mother and child. However, if the mother is RH- and the father RH+, there may be issues, in the sense that the baby may inherit the father’s RH+. In this precise case, the mother can manufacture anti-rhesus (antibodies) to combat the molecule and risk sending it to the baby through the placenta.
The passage of the mother’s antibodies in the fetal blood can lead to anemia, swelling, jaundice and brain damage in the fetus. When this blood incompatibility is screened for early in the pregnancy, the mother will receive a vaccine around 28 weeks pregnant. The WinRho vaccine neutralises the formation of antibodies and stops this fight reaction, a rejection that might occur.
Search for Antibodies:
To know if a mother is immune from certain illnesses, we search for antibodies in her blood which tells us if she is protected or not. The typical example we use is varicella (chickenpox). When a person has had chickenpox or had the vaccine, generally they are immune, are defended against the virus. So during pregnancy, we will look for anti-varicella, antibodies that provide protection. The same applies for hepatitis B, C (not automatic for all mothers), rubeola, parvovirus B-19 (5th disease) and HIV (Human Immunodeficiency Virus).
About 60% of people will become immune to parvovirus B-19 during their life, but infection is asymptomatic in most cases. The mother-fetus transmission during pregnancy can take place in 17-33% of cases if not immunised, but for most there are no consequences after the first trimester. The virulence is felt more in the home (50%) and daycare or school (20-30%).
The influenza vaccine during pregnancy is not a vaccine that lasts for years and needs to be repeated every year to protect the person. Public health officials recommend that pregnant women get vaccinated, as there are more benefits than risks from the vaccine. This is to prevent complications such as early labour during the 3rd trimester, fever, pneumonia and hospitalisation for care. The injectable vaccine is inactive, so there are no risks for the fetus. Never take the inhalable vaccine, as it is living and is often given to young children.
Why?
If a mother is not immune to an infectious disease which can be severe during pregnancy, some vaccines can be recommended, for example, hepatitis B. If they aren’t available, they will increase prevention. That’s why it’s always good for women who are at the age to procreate visit their doctor before conceiving. They will be screened to receive antiviral treatments if infected and/or vaccines to avoid exposing the baby to the virus in utero. It also helps avoid adverse impacts on childbirth.
There are a variety of potential complications associated with infection by these viruses during pregnancy. They can lead to fetal malformations, neurological or ophthalmic (vision) disorders, growth disorders, immunity disorders, miscarriages and even extend to fetal death in the most extreme cases.
Toxoplasmosis
Toxoplasmosis is a disease caused by a parasite called the Toxoplasma Gondii.
The infection symptoms in a pregnant woman often go unnoticed, as they resemble the signs of severe flu: fever, sore throat, muscle pain.
This parasite can be contracted through exposure to cat excrement, raw or undercooked meat and raw milk.
Why?
The toxoplasmosis parasite can be transmitted to the fetus. Infection is more frequent at the end of pregnancy and has fewer risks for the baby. However, if the infection occurs at the start of pregnancy when cells are developing exponentially, the damage to the baby may affect their sight, hearing, and nervous system leading to intellectual delays.
Rapidly screening for toxoplasmosis allows us to treat the mother with antibiotics to prevent potential complications.
Please read my article about toxoplasmosis.
Lisez mon autre billet sur la toxoplasmose.
Infectious Syphilis (VDRL):
Infectious syphilis is a sexually transmitted blood-borne disease that can affect several body systems. The risk of transmission to the baby during pregnancy for an untreated woman is around 70 to 100% for a primary infection. This risk drops to around 40% if the infection is considered latent (past contamination). However, congenital syphilis (transmitted intrauterine) can be prevented easily with early treatment of the pregnant woman.
Why?
Infectious syphilis in pregnant women predisposes them to miscarriage and premature delivery.
As for the baby, if left untreated, it too is at high risk of infection. Although 20-60% of newborn babies remain asymptomatic, the remainder may develop rashes on the palms and soles, often in the form of blisters, mostly within the first two months of life. It can also cause growth retardation and fetal malformations.
The INSPQ is currently working on the 2023 update, and statistics show that the rate of syphilis infection in women rose by 198% between 2016 and 2020. In the future, systematic screening may also be introduced in the last trimester of pregnancy, to improve detection and intervention.
Screening Test for Gestational Diabetes
The screening test for gestational diabetes is usually done around the 28th week of pregnancy to prevent related potential complications up to childbirth. However, your health professional might ask for the test at the start of pregnancy if there are risks factors involved:
- The mother’s age (over 35)
- The mother is overweight
- Previous gestational diabetes during a previous pregnancy
- Close members of the family with type-II diabetes
- The mother already gave birth to a very big baby
- The mother has polycystic ovaries
The test consists of drinking a sweet juice containing 50 g or 75 g of glucose. You will then have a blood test.
Why?

Early screening of gestational diabetes can completely change the whole pregnancy and outcome. Once it’s diagnosed, health professionals will increase their monitoring with closer medical appointments, more ultrasounds and preventative measure associated with diet, exercise and regular sugar measurements.
The risks for the baby are mostly associated with different malformations depending on the stage of pregnancy. Often the baby will be bigger at birth, and there may be other pulmonary, neurological and kidney complications.
The mother risks miscarriages, hypertension (high blood pressure), vision issues. These mothers often give birth prematurely or by caesarean section.
Obesity Evaluation:
This check-up is done when a pregnant woman is considered obese or morbidly obese. Her BMI is way above her healthy measurement. Instead of a BMI between 18.5-24.9, the mother may have a measurement above 35.
Besides this fact, at the start of pregnancy, your health professional may request tests for kidney function (relating to the normal work by your kidneys) and hepatic function (referring to the liver and blood calculation of its enzymes). These are to examine for potential dysfunctions as early as possible.
Why?
During pregnancy, the woman’s increased metabolism brings out already present problems. Also, if they already know the measurements, your health professionals can suggest appropriate treatments or monitoring based on your situation to reduce the consequences as much as possible, both for the mother, the pregnancy and the baby.
Hemoglobin Electrophoresis:
Hemoglobin electrophoresis is a test used to screen for a disease that affects hemoglobin quality in the blood. It distorts the red cells (which transport iron in the blood) and can cause a type of anemia known as iron deficiency anemia.
This occurs mainly in mothers who are not of North American origin. It affects many African mothers. By screening for this problem early, we can provide the mother with higher amounts of iron.
Why?
If the problem isn’t screened for and it persists, the mother is at a higher risk of iron deficiencies and develop urinary infections. She may have more preeclampsia (increased blood pressure, proteins in her urine, swelling of her appendages) and often give birth prematurely.
For the baby, this situation can lead to low birth weight and different infections after childbirth.
As you can see, many blood tests can be requests from the start of pregnancy. Your health professional will choose them based on your health and life history.
I hope this article has helped answer some of your questions and understand the need for these tests.
Talk soon,
Marie
The Baby Expert


