Being diagnosed with gestational diabetes, also known as pregnancy diabetes, scares many future fathers and mothers. Diabetes that occurs during pregnancy affects 3% to 9% of pregnant women.
This article provides clarifications in layman’s terms but does not deal with women who were already diabetic before their pregnancy, as the explanations are not totally the same.
What is gestational diabetes?
Like you already know, pregnancy comes with a lot of changes in a woman’s body. She is now carrying a small being that is growing and developing. Her body needs to adapt to this demanding renter to provide it with everything it needs.
The World Health Organisation defines gestational diabetes as a glucose tolerance disorder, of variable severity, emerging or diagnosed for the first time during pregnancy.
From 3% to 9% of pregnant women will be diagnosed with pregnancy diabetes, and this percentage varies if you look at data from American, Canadian sources and the Society of Obstetricians and Gynecologists of Canada (SOGC).
The First Trimester of Pregnancy
Just like for many systems, pregnancy hormones (estrogen and progesterone) will have an impact on the regulation of blood sugars in pregnant women. It destabilized the balance with the secretion of available insulin. Insulin is a hormone secreted by the pancreas which manages the balance with glucose (or blood sugar). In other words, insulin neutralises blood sugar. That said, in general, from the start of pregnancy, there is an increase in the release of insulin associated with hormonal changes. This reduces blood sugar (glucose), and this explains why a newly pregnant woman can feel signs of hypoglycemia, such as:
- Fatigue;
- Dizziness;
- Hunger;
- Thirst;
- Irritability.
You should also know that sugar is the primary fuel for the development of the fetus in utero, and this sugar comes from the mother via the placenta.
However, the mother’s insulin cannot pass through the placenta to the baby. Starting at around ten weeks, the baby will produce their own insulin to manage its mother’s glucose.
If the blood sugar (glucose) levels increase in the pregnant woman, it will also increase in the same way for the baby. This glucose level will force the baby to work harder to secrete enough insulin to maintain the proper balance.
Second and Third Trimester of Pregnancy
When the second trimester arrives, we note that pregnancy hormones increase their effect on the pancreas producing resistance to the release of insulin. In other words, the hormones counteract the effect of insulin neutralising blood sugar. There will then be an automatic increase in glucose in the pregnant woman’s body.
This occurs automatically in all pregnancies, and the goal is to provide the fetus with a high level of sugar to ensure its growth. However, the future mother’s body will adjust, producing up to three times the average level of insulin to compensate for the blockage caused by the pregnancy hormones.
In the vast majority of cases, the pregnant woman’s pancreas can secrete sufficient amounts of insulin to maintain an acceptable balance between glucose (sugar) levels and insulin. There are few cases where the pancreas cannot meet the demand, but when this occurs, gestational diabetes will be diagnosed.
Gestational Diabetes Screening Tests
 The screening test for gestational diabetes usually takes place between 24 and 28 weeks of pregnancy. Most women will take the 50 g test drinking a very sweet orange juice. The juice contains 50 g of glucose and rapidly increases the sugar level in the blood. One hour later, a blood test will be done to check how the pancreas reacts and increases insulin production due to the increased glucose.
The screening test for gestational diabetes usually takes place between 24 and 28 weeks of pregnancy. Most women will take the 50 g test drinking a very sweet orange juice. The juice contains 50 g of glucose and rapidly increases the sugar level in the blood. One hour later, a blood test will be done to check how the pancreas reacts and increases insulin production due to the increased glucose.
The test doesn’t have to be done on an empty stomach.
Due to the drastic change in blood glucose, some women may feel unpleasant symptoms, such as nausea and sometimes vomiting, reflux, increased heartbeat and even feeling like they will pass out.
When the results are within normal values (between 7.8 and 10.2 mmol/l, which may vary depending on the medical team), the pregnant woman does not have gestational diabetes, and her pancreas is managing the balance between glucose and insulin.
However, if the glucose remains higher than it should (above 10.2 mmol/l or different target based on the medical team), they may suggest that she pass the oral glucose tolerance test (OGTT) test, which diagnoses pregnancy diabetes.
Gestational Diabetes Diagnostic Test
The diagnostic test for gestational diabetes is called an Oral Glucose Tolerance Test (OGTT). The pregnant woman will drink juice with a dose of 75 g or 100 g of glucose (depending on the medical prescription). Then two blood tests will be taken one and two hours after drinking the liquid. This is to verify if the woman’s pancreas produces enough insulin to combat the sudden increase in glucose.
Usually, pregnant women take the OGTT test on an empty stomach while maintaining their regular diet and activities for the three days before the test. Note that caffeine naturally increases glucose.
The three-hour OGTT test will diagnose if a woman has gestational diabetes or not. If there are two measurements above normal levels, gestational diabetes will be diagnosed. Measurement examples:
- If glucose on an 8-hour empty stomach is above 7 mmol/litre
- If after two hours post-75 g glucose test the result is above 11.1 mmol/l
- If glucose, irrespective of meals, is above 11.1 mmol/l
On the other hand, if there is only one higher measurement, this is more glucose intolerance.
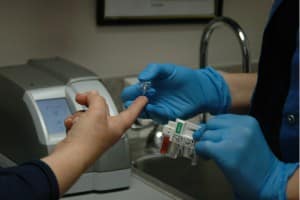
A blood glucose test is also possible. When a pregnant woman is offered a blood glucose test, they have to be taught how to prick their finger four times a day for one week, on waking and then one hour after every meal. The mother will note the measurements in a notebook, and then the health professional will check the results to ensure that they are between 3.5-5.2 mmol/l on waking and not above 7.1-7.7 mmol/l after meals.
This allows us to check a larger week-long sample to understand daily glucose fluctuations better.
Classifying Gestational Diabetes
Gestational diabetes is classified into two types. The two types do not correspond to those for women who were diabetic before pregnancy. Here are the explanations for types A1 and A2:
Type A1
Type A1 gestational diabetes refers to a pregnant woman who had one or several results outside of usual standards during the OGTT test but has normal glucose levels on an empty stomach. In this case, your doctor or nurse, endocrinologist or nutritionist will monitor you to help you balance your meals to stabilise your glucose for the rest of the day.
In most cases, a proper diet is enough, and it will be adjusted as the pregnancy moves forward. This includes handling the growing resistance to insulin in the woman’s body.
Type A2
Type A2 gestational diabetes affects 20% of pregnant women who have pregnancy diabetes. They must take medication to maintain their glucose levels. For this type, dietary modifications are not enough to stabilise the situation.
Treating and Monitoring Gestational Diabetes
Treating and monitoring gestational diabetes takes place at many levels.
1. Diet:
Your diet is the most important consideration when treating gestational diabetes. A nutritionist will help you calculate your recommended calories consumed per day based on your age, weight, history, glycemia results, etc.
2. Exercise:
Exercise helps reduce blood glucose in pregnant women because muscles use sugar when active. This lowers the insulin demand.
Being active helps control glucose during pregnancy. Aerobic and muscle exercises should be part of your daily routine.
3. Measuring Blood:
Taking four blood glucose tests per day allows you to monitor the balance between sugar and insulin in your blood. Often this is done in the morning on an empty stomach then one hour after a meal. It can be more frequent, based on each person’s situation.
4. Treatments with Medication:
For women who need it, oral or injected insulin medications might be necessary to maintain your blood glucose balance and prevent possible complications.
5. Monitoring:
- Fetal monitoring at least twice a week starting from 32 weeks pregnant.
- Frequent ultrasounds to monitor the baby’s weight
- Possible induction before 40 weeks, to prevent possible complications at the end of the pregnancy
- A caesarean will be planned only if the mother’s condition does not allow for vaginal childbirth.
Protective factors for screening gestational diabetes
- Under 25
- Caucasian
- A BMI under 27
- No gestational diabetes history in the family, or intolerance to glucose
- No history of diabetes in the immediate family (father, mother, brother, sister).
Risk factors for developing gestational diabetes
- Over 35
- BMI over 30
- Known to have polycystic ovaries
- Giving birth to a very large baby (macrosomia)
- Being treated with certain medications
- Part of high-risk populations (Hispanic, Asian, African)
Possible Complications of Gestational Diabetes
The possible complications due to gestational diabetes can affect both the mother and baby.
For the baby:
- More congenital anomalies when there’s pre-existing diabetes (before the pregnancy), such as 7% to 10% of cardiac malformations, cardiomyopathy, musculoskeletal and neurological disorders. But in the case of gestational diabetes, there seem to be no risks for congenital anomalies given diabetes frequently emerges near the end of the pregnancy and the baby in advanced development in utero.
- Frequent hypoglycemia in the period after birth
- Respiratory problems at birth
- Risk of 1/3 recurrence at next pregnancy
- In 15% to 30% of cases, macrosomia, meaning a baby that is bigger than average
- More traumatic childbirth given the weight of the baby
- Premature birth
- Jaundice
- In utero death (very rare case given monitoring)
Later in life:
- Obesity
- Diabetes
For the mother:
- More amniotic fluid (polyhydramnios)
- Risk of high blood pressure and preeclampsia
- Risk of obesity later in life
- In 10% to 60%, more risk of developing diabetes within the next 20 years
Postnatal Monitoring
The new mother’s glucose will be monitored for 6-12 weeks after childbirth or after they stop breastfeeding. The woman will take the 75 g glucose test (OGTT) again to ensure that her blood parameters are back to normal.
In conclusion, pregnancy diabetes is a complex issue. This article aimed to provide helpful information on the topic without delving too deeply into the medical or biological aspects. When a future mother receives uncertain or challenging glucose test results, a support team will be available to offer guidance and encouragement throughout the pregnancy and beyond.
As always, it is important to make every effort to ensure that the situation unfolds as smoothly as possible for everyone involved.
Marie Fortier
The Baby Expert
Article updated on january 2021.