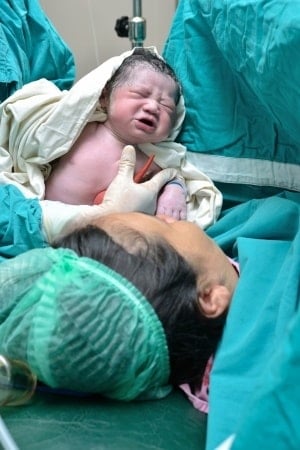
Caesarean section is another way of delivering a baby, and it’s essential to talk about it during childbirth preparation, since it’s a possible scenario, for a variety of reasons.
We know that well-prepared parents are calmer, better able to understand the context, the indications and, above all, the risks associated with having or not having a Caesarean section. There are several contexts in which a C-section is required: emergency, elective (planned in advance) and during labor. A gynecologist or surgeon will perform the operation.
We know that well-prepared parents are calmer, better able to understand the context, the indications and, above all, the risks associated with having or not having a Caesarean section.
According to Canadian statistics, nearly 28%* of deliveries will be by C-section. (*SOGC, 2019.)
A Caesarean section is a surgical procedure that allows the birth of one or more babies via the abdominal route when a vaginal delivery cannot be performed, or in an emergency situation.
Emergency C-section
An emergency Caesarean section is usually performed within minutes of an observed situation. For example, bleeding related to placental abruption or placenta previa (placed in the cervix), a worrying drop in the baby’s heart rate, or cord prolapse (the cord descends in front of the baby’s head into the mother’s pelvis). In such circumstances, time is of the essence! In such cases, the father or other significant person may not be invited to be present in the operating room, given the speed of the operation and the high level of attention and concentration required of the mother and baby. What’s more, if the woman giving birth is not already anaesthetized, she may have to be put to sleep to speed up the procedure and get the baby out quickly.
Planned caesarean section
The context of planned (iterative) caesarean section refers more to health situations experienced during pregnancy, to reasons known in advance for considering this surgery even before a trial of labour. Here are a few common examples: the placenta is in the wrong place, the baby is too big, the baby is breech… It may also be related to a condition in the mother, such as a physical problem (e.g. fibroid, herpes sore on the vulva), a chronic illness (e.g. poorly controlled diabetes) or a previous Caesarean section.
The advantages of a planned cesarean section can be summarized as follows:
- Avoid unnecessary labor;
- Eliminate the fear of vaginal delivery;
- Know your due date in advance;
- Less trauma to the pelvic floor;
- Avoid caesarean section during labour.
When a C-section is planned, you may be offered a preparatory meeting before the procedure.
Alternatively, a C-section may be neither planned nor urgent, but may still be necessary in certain circumstances. For example, a caesarean section may be performed during labour if there is a stoppage of progress (the cervix is not changing), suboptimal positioning of the baby that prevents its descent into the pelvis, ineffective contractions, a fetal heartbeat with significant decelerations after contraction, etc.
Caesarean section procedure
The surgery will involve inserting an intravenous solution and a urinary catheter, administering anesthesia (epidural, spinal or combined epidural and spinal anesthesia), monitoring vital signs and then making a horizontal cut just above the pubic bone to gain access to the uterus. The woman’s bladder will first be emptied with a urinary catheter, which will remain in place throughout the operation to avoid being traumatized in the process. Most women undergoing Caesarean section will remain awake during surgery, thanks to a regional anaesthetic. It is very rare for a mother to be put to sleep to deliver the baby, but it is sometimes necessary to do so in certain situations.
The surgery itself takes about 45 minutes, and the post-surgery monitoring period lasts about an hour and a half. Convalescence time after a C-section is about 6 weeks. You should therefore plan to have help at home for the first 2 or 3 weeks, so that the mother can devote herself to her own recovery and the care of her baby, as she slowly resumes her daily routine.
Marie Fortier
The Baby Expert
Updated article : October, 2024.
For more information about the subject, read the following articles :
- Experiencing a caesarean
- Forceps or cesarean
- The realities of childbirth
- Why take prenatal classes?
- Let’s talk placenta
- Epidural or spinal anesthesia
Also, watch these videos :