Updated article on June 6, 2023.
Trisomy 21 (also called Down’s Syndrome), 18 or 13 are different types of trisomy that refer to problems associated with chromosome configuration. These chromosomes carry genes that will be transmitted to the baby’s genetic code. A chromosomal dysfunction can lead to different repercussions for the future baby’s physical and mental health. But it is impossible to determine these impacts before the baby is born, grows and develops.
In Quebec, approximately 1/770 children will be diagnosed with Down’s Syndrome out of 87,000 births.
The screening is entirely voluntary and consists of 2 blood tests taken from the future mother at two different times, to measure the most common aneuploids. The first test needs to be done between the 10th and 13th week of pregnancy, and the second between the 14th and 16th week of pregnancy to obtain the best results.
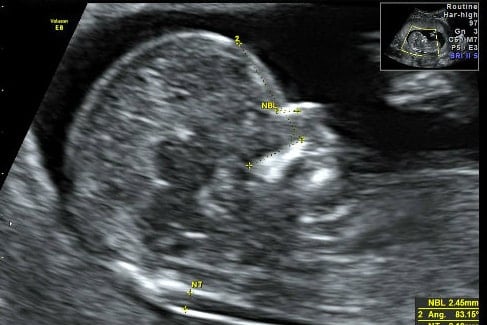
The results of these measurements do not diagnose trisomy. They indicate the risk of giving birth to a baby with Down’s Syndrome. The detection rate is around 80-85% with a margin of error. Some pregnant women, in addition to screening tests, will have what is called a nuchal translucency ultrasound at 12 weeks of pregnancy. It measures the fluid at the back of the baby’s neck, which increases measurement reliability and improves the detection rate to more than 95% with a tiny margin of error. The nuchal translucency ultrasound is not universally offered in the health network. It is provided by many private clinics, available to parents who want to take it. Even a dating ultrasound can increase the screening detection rate from blood tests.
According to the SOGC clinical directives, all pregnant women in Canada should be given prenatal screening tests. In the best of worlds, a fetal ultrasound between the 11th and 14th week of pregnancy should be part of these tests. This ultrasound also allows health professionals to evaluate fetal viability, gestational age (dating), the number of fetuses, early anatomy and nuchal translucency depending on the options offered.
Over recent years, private companies as at Prenato have started offering other tests to screen for trisomy 21, 18 and 13, using acellular DNA analyses of the mother’s blood. The test is safe for both mother and baby. It is highly effective, but not generally available to all women given the high cost of performing it. Regardless of the mother’s age, if a parent wants to be as certain as possible of detecting potential pathologies in their fetus, which can now be identified on DNA, it’s better to choose this type of test rather than the tests provided by the health network, which are much less specific in their conclusions.
The DNA test studies the baby’s free cells in the placenta, also present in the mother’s blood, providing information on the fetus’s genetic code as early as 10 weeks into the pregnancy. Not only can we know the baby’s exact sex, but much more besides. DNA can also be used to identify other genetic diseases such as cystic fibrosis, sickle cell anemia, Duchenne muscular dystrophy and more.
With today’s technology at Prenato, there are also several syndromes that can result from fetal DNA testing, which highlights a lack (deletion), mutation or disorder of the chromosomes on the gene, leading to various possible dysfunctions in the fetus to come. Prader-Willi, Angelman and Wolf-Hischhorn syndromes, not to mention Cri du chat and Di George, can now be identified during pregnancy using a fetal DNA test.
The detection rate is 98-99% and costs are around $500 to $800. Parents have to pay the full price, but many insurance companies reimburse these expenses.
It is important for parents to be informed in order to make an informed choice, since a parent could knowingly ask his or her doctor for a prescription for a private fetal DNA test as early as the first trimester of pregnancy.
If the screening test results indicate a high trisomy risk, your health professional will help you choose the best possible option. If you want to have further screening tests, you have two options. The first is an amniocentesis (removal of amniotic fluid and fetal cells with a needle) for more in-depth analysis. The second is chorionic villus sampling, where the baby’s chromosomes will be examined from a small sample of the placenta.
Research is ongoing for tests that don’t require the use of a needle. Known as NIPS (non-invasive prenatal genetic screening), it involves taking a blood sample from the mother. Her DNA, as well as DNA from the placenta (which includes fetal DNA (5-15%)), is isolated. Technicians can validate the presence of trisomy risk with a false negative margin of error of about 0.5-1%, which is very respectable.
I know that it’s not easy for parents to know what is best for them in a case like this. But I hope the information they receive from health professionals at the start of their pregnancy can help them make informed decisions. Always ask questions, get the answers you need, and then decide together.
I hope this article has been helpful.
Talk soon,
Marie
The Baby Expert